Osteoarthritis is a chronic disease in which the structure of the connective tissue of the musculoskeletal system is damaged. The disease is characterized by a progressive course, against the background of which the cartilage tissue is gradually destroyed. This pathology is diagnosed in many people over the age of 65 because one of the factors that contribute to the development of this condition is the natural aging process in the body.
Description of the disease
A post-traumatic, endocrine and inflammatory disease, excessive physical overload or, on the contrary, inactivity can provoke the development of a degenerative-dystrophic disease. The main signs of osteoarthritis: pain in the joint area with edema and limited activity.
To diagnose the disease, they resort to instrumental techniques - X-ray, arthroscopy, CT and MRI. In the treatment of stages 1 and 2 osteoarthritis, conservative methods are used - taking medication, physiotherapy, massage and physiotherapy. If irreversible destructive changes in the joint tissue have occurred, then surgery is required - arthrodesis or endoprosthetics.
Pathogenesis
Osteoarthritis is characterized by pronounced changes in the structure of the connective tissue. The formation of deforming erosions occurs on the cartilage, which destroys collagen fibers and proteoglycans, which contain protein (5-10%) and glycosaminoglycans (90-95%).
As a result, the stability of the collagen network decreases, metalloproteinase is released and all protein forms in the extracellular matrix are destroyed. The acceleration of the destruction occurs due to the fact that the biosynthesis of collagenases and stromelysin increases.
When enzymes are present in normal amounts in the body, they usually keep the levels of cytokines - small peptide information molecules - under control. As osteoarthritis progresses, the concentration of this protein decreases, releasing enzymes that affect cartilage in a large volume.
Proteoglycans with a distorted structure therefore absorb water that they cannot hold back. Because of this, excess fluid penetrates the collagen fiber, which begins to "swell", resulting in a loss of strength and elasticity.
The qualitative and quantitative composition of the synovial fluid also deteriorates. Against the background of osteoarthritis, a decrease in the concentration of hyaluronic acid is observed in it. The transport of nutrients and oxygen to the hyaline cartilage tissue stops in the volume necessary for its recovery. Softened foci are formed in the cartilage, followed by the formation of cracks, specific necrotic growths. Then the bare heads begin to be exposed, microtrauma appears against the background of displacement to each other.
What provokes the development of the disease
Why primary (idiopathic) osteoarthritis develops has not yet been clarified. Such a disease develops without the influence of factors, so doctors believe that the cause of such a problem lies in the tendency at the genetic level to premature destructive processes in cartilage. The formation of secondary osteoarthritis occurs as a complication of other joint diseases or against the background of an injury.
The presence of the following factors can lead to the formation of degenerative-dystrophic pathology:
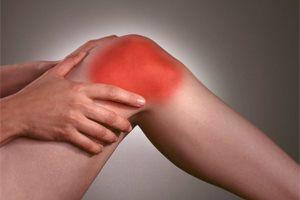
- Damage to the joint tissue or in the vicinity of the connective tissue structure in the form of a fracture, dislocation, meniscus injury, partial rupture or complete separation of muscle and ligament tissue, tendons;
- congenital dysplastic disorder in the development of joints;
- Disorders in the functionality of the endocrine glands, metabolic disorders;
- rheumatism or rheumatic fever;
- Polyarthritis, rheumatoid, reactive, metabolic, gouty or psoriatic arthritis;
- purulent arthritis, the cause of which lies in the effects of streptococci, epidermis or Staphylococcus aureus;
- tuberculosis everywhere, brucellosis, chlamydia, gonorrhea, syphilis;
- degenerative-dystrophic pathologies, for example osteochondritis dissecans.
The increased mobility of the joint tissue, which is observed against the background of the production of special collagen fibers in the body, can contribute to the formation of osteoarthritis.A similar phenomenon is observed in 10% of people living on the planet. It is not considered a disease.Although against the background of hypermobility there is a weakness in the tendon-ligament system, due to which a person is prone to injuries, especially in the ankle, in the form of sprains and ruptures of the ligament tissue, dislocations.
In some cases, problems with haematopoietic function (for example, the presence of haemophilia) can lead to the formation of osteoarthritis. Against the background of hemarthrosis (bleeding into the joint cavity), the blood supply to the cartilage tissue deteriorates, as a result of which it begins to collapse.
Among the predisposing factors, it should be noted the presence of age, frequent loads on the articular tissues that exceed the limits of its strength, excessive body weight, performed operations and hypothermia.
The risk group includes women going through menopause, citizens who live in adverse environmental conditions or come into contact with toxic chemicals. When the diet does not contain enough vitamins and minerals, conditions arise for the gradual destruction of hyaluronic cartilage tissue.
Symptoms

Osteoarthritis is dangerous because the first stage of formation is asymptomatic. The manifestation of the clinical picture occurs over time, the primary symptoms appear with a significant destruction of the cartilage.First of all, the patient feels a slight pain syndrome without a clear localization.It occurs after physical exertion - lifting heavy objects, sports training.
In some cases, the first sign a person notices the appearance of crunches and clicks during the flexion or extension of the joints. The patient notes that it is sometimes difficult to move. Although in the early stages of osteoarthritis, mobility problems do not appear until the morning and go away quickly.
With the advancement of pathology, painful sensations begin to interfere at night, as a result of which the sleep function is disturbed, and chronic fatigue also occurs. As the disease progresses to grade 2, the intensity of pain increases against the background of changes in weather conditions, exacerbations of chronic diseases and acute viral infections of the respiratory tract.
The physical activity decreases significantly. Mobility is hindered by the thinning of the cartilage tissue and the patient's deliberate restriction of movement in order to prevent pain. This increases the stress on the tissue of the opposite joint, which contributes to its further destruction.
Osteoarthritis is characterized by other specific features:
- Pain, which provokes the appearance of spasms in the skeletal muscles and the formation of muscle contractures (impaired passive motor function of the joint);
- crunching in the joint tissue, clicking, crackling during a movement of a constant nature that occurs practically with every displacement of bones in relation to one another;
- frequent painful muscle cramps;
- deformation of the joints, which leads to impairment of posture and gait;
- pronounced deformity up to the curvature of the joints with a significant decrease or complete absence of motor activity in them against the background of 3rd degree osteoarthritis.
If osteoarthritis of the knee, ankle, or hip has developed by stage 3, a person must use a cane or crutches when moving.
If you do not start treatment on time, the disease will begin to progress, relapses are a regular bother you, and exacerbations will become more frequent over time. The stiffness in the morning hours does not go away for long, but gradually becomes permanent.
When examining a person with stage 1 osteoarthritis, the doctor only finds slight edema of the joint tissue, whereby the motor function is fully preserved. Stage 2 of the disease is manifested by pain and slight deformities on palpation. Bone thickening forms near the synovial cavity.
Osteoarthritis is characterized by the formation of synovitis - inflammation of the synovia in the hip, ankle, knee or shoulder joint. The main symptom of this disease is the development of a rounded seal near the joint. When you press it, you can feel the contents of the fluid move. With acute synovitis, the temperature can rise to 37-38 degrees, headaches and digestive problems can appear.
Diagnostic measures
The disease is diagnosed based on the results of the study using instrumental methods, clinical features, anamnestic data and patient complaints. In this case, a clinical examination of blood and urine is not very informative - all indicators remain in the normal range, if the cause of osteoarthritis is not in metabolic problems.
When synovitis develops, the sedimentation rate of erythrocytes increases (up to 30 mm / h), the leukocytes and fibrinogen in the blood increase.This indicates the presence of acute or chronic inflammation in the body.Biochemical and immunological parameters change with osteoarthritis of the secondary form.
The most informative way to identify degenerative-dystrophic diseases is to take an X-ray in two projections (lateral and straight).
On the X-ray, the osteoarthritis is shown as follows:
- In the initial stage there are no radiological signs.
- In the first stage, the pathology is presented as an indistinct, uneven narrowing of the joint cavity. The edges of the bone plates are slightly flattened, initial osteophytes are formed (sometimes they are absent).
- In the second stage, the picture shows an image in the form of a pronounced narrowing of the cavity in the joint, which exceeds the norm by 2-3 times. Osteophytes are formed in large numbers, the formation of subchondral osteosclerosis is noted. Cyst-like illuminations appear in the appendages.
- In the third stage, the picture shows pronounced subchondral osteosclerosis and large marginal osteophytes. The joint space is significantly narrowed.
- In the fourth stage, coarse massive osteophytes are formed, the joint space is almost completely fused, the bony appendages that form the joint are deformed and compacted.
If the doctor has doubts about the diagnosis after examining the x-rays, the patient will be prescribed a computed tomography. An MRI is done to assess the condition of the connective tissue near the joint. By using a contrast agent, you can follow the dynamics of how tissues are supplied with blood to determine the degree of inflammation in synovitis.
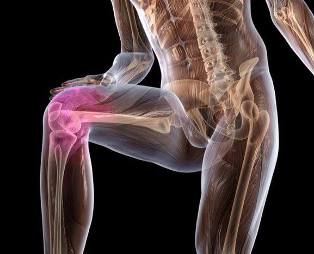
Treatment of osteoarthritis
A complete cure of osteoarthritis is currently not possible as there are no pharmacological agents that restore the cartilage tissue.The main goal of treatment is to prevent the further development of the disease and to keep the joints flexible.Treatment of osteoarthritis is long-term and complex and involves the use of local and systemic drugs.
Patients should not overload their joints. Motor activity must be limited with the help of orthopedic devices - orthoses, elastic bandages. Obese people need to adjust their diet in order to lose weight over time and begin dieting.
When stable remission is achieved, the patient must do therapeutic gymnastics every day. First you need to do this under the supervision of a specialist, and in the future you will need to do gymnastics yourself at home. In addition to physical therapy, you can sign up for the pool, do yoga, or ride a bike.
To reduce the intensity of pain, the use of drugs is prescribed that belong to different pharmacological groups:
- Nonsteroidal anti-inflammatory drugs in tablets, ointments and solutions for intravenous injections.
- Intra-articular injections of anesthetics with the addition of glucocorticosteroids.
- Muscle relaxants to relieve muscle spasms and contractures.
The treatment regimen for osteoarthritis also includes the use of B vitamins, sedatives, if necessary - antidepressants and sedatives. It is mandatory to appoint chondroprotectors in the form of a long course.Means of this group contribute to the partial restoration of the cartilage.
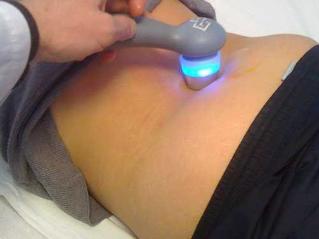
In order to increase the clinical activity of the joint tissue, it is necessary to carry out physiotherapeutic procedures - laser therapy, magnetotherapy, UHF.
Painful manifestations in the area of the joints should be the basis for an immediate doctor's visit. Treatment in the early stages of osteoarthritis development makes it possible to stop destructive processes in the cartilage to prevent disabilities and disabilities.



























