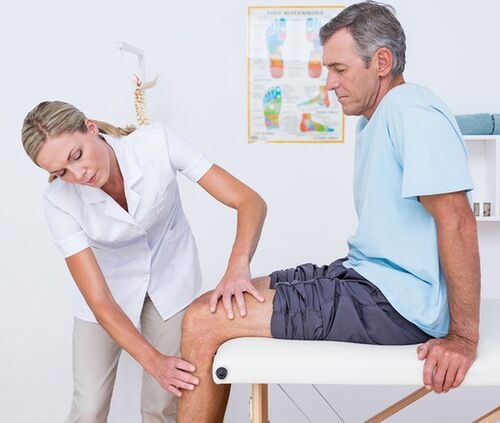
Knee pain- This is a sign of pathological processes affecting the cartilage, bone or soft tissue structures of the femoral-tibial and femoral-patella joints. Arthralgia can be due to trauma, inflammatory and degenerative diseases of the joint apparatus and the periarticular structures. Patients may complain of sharp, sore, burning, throbbing, and other types of pain that occur at rest or when moving, supporting, bending, and extending the leg at the knee. The diagnosis of causal pathology includes instrumental imaging methods (Rg, ultrasound, CT or MRT, arthroscopy), puncture of the joint capsule, biochemical and immunological analyzes. Until the diagnosis is clarified, rest, immobilization of the joints, NSAIDs, and analgesics are recommended.
Causes of knee pain
Traumatic injury
Usually they are the result of household trauma that is common in athletes: runners, jumpers, athletes. Caused by a fall, direct impact or twisting of the leg. Manifested by sharp pain at the time of injury. In the future, the pain syndrome will become less pronounced, accompanied by increasing edema. Abrasions and bruises are possible. With increasing frequency, the following injuries are identified:
- Knee injury. . . Occurs when you fall on or hit your knee directly. At first the pain is sharp, hot, sometimes burning, but bearable, later - dull, aching, aggravated by movements. Bruising is possible. The legrest is retained. Sometimes a knee injury is complicated by hemarthrosis, in such cases the joint gradually increases in volume, becomes spherical, a feeling of pressure or bursting is added to the pain syndrome.
- Tape tear.It is found in an unphysiological position after twisting the leg, forcibly twisting it, bending it, or hyperextending it. The painful sensations are stronger than with a bruise; at the same time as the onset of pain, a person may feel something being torn (similar to ordinary tissue). It is accompanied by significant restriction of movement, support, twisting of the limbs, and rapidly increasing hemarthrosis.
- Intra-articular fractures. . . They are recognized by bumps, falls, and twisting of the leg. When injured, a person feels a very sharp, often excruciatingly sharp pain, sometimes a crunch can be heard. Even patients with intra-articular fractures describe their feelings as follows: "The pain is such that it darkens in the eyes, the world ceases to exist, one does not understand anything. " Then the pain becomes less severe but remains of high intensity. Support is usually not possible and movement is almost completely restricted. Edema and hemarthrosis progress quickly.
- Dislocation.Is the result of a blow or fall on the knee. At the time of patellar dislocation, there is a sharp pain, accompanied by a feeling of flexion of the leg and displacement in the knee. No movement possible, the reference function can be saved. A pronounced deformation is visible on the front of the knee, which is subsequently smoothed out by the increasing edema. Sometimes this is followed by hemarthrosis.
- Pathological fractures.They develop with minor injuries, are a consequence of a decrease in bone strength in osteoporosis, osteomyelitis, tuberculosis, bone tumors. The pain is painful, dull, reminiscent of the pain syndrome with a bruise. Signs of a pathological fracture are limitation or inability to support the leg, a feeling of instability in the knee, sometimes deformity, bone crunching during movement.
- Damage to the menisci.Meniscus tears arise from twisting, impact, intense forced flexion or extension of the knee, sharp rotation with a firm leg. At first, a person feels a special click and sharp, stabbing pain in the depths of the joint. Then the pain subsides a little, but becomes diffuse, sometimes - burning, bursting, intensifies when trying to support and move. The knee volume increases due to edema and hemarthrosis. Support becomes impossible, movements are severely restricted.

Inflammatory diseases
They can be infectious and non-infectious (post-traumatic, toxic-allergic, metabolic, after vaccination). An abundant blood supply to the synovial membrane and periarticular tissue promotes the rapid development of inflammation in response to direct and indirect effects, and a large number of nerve endings cause a marked pain response. The inflammatory process is often accompanied by synovitis (accumulation of aseptic fluid in the joint), with an infection, pus can accumulate.
- Arthritis.Gonarthritis occurs after injuries, sometimes complicates infectious diseases and is detected in rheumatic diseases. Can be acute or chronic. Knee pain is usually dull, aching, pressing, or pulling. The pain is initially not intense and intermittent, but intensifies in the evening or after training. Then the beginning pain joins, the intensity and duration of the pain syndrome increases. The joint swells, the skin over it turns red, the temperature rises. With synovitis, the contours of the knee are smoothed, creating a feeling of bursting. With suppuration, the severity of the pain increases sharply, they become twitching, deprive of sleep.
- Synovitis.It is not an independent disease that complicates many acute and chronic pathologies of the joint. It is formed within a few hours or days. At first the pain is insignificant or absent, there is a feeling of fullness. The knee is spherical, with a lot of fluid, the skin is shiny. Movement is somewhat restricted. With an infection, the pain becomes pronounced, pulsating, twitching, intensified with the slightest movement and touch.
- Bursitis.Inflammation of the joint capsules located in the kneecap and the hollow of the knee usually occurs when the knee is overloaded and the injuries are repeated (e. g. with constant support on the knees). With bursitis, the pain is local, dull, not intense, occurs in a certain position of the limb, after a characteristic load it decreases when the position of the leg changes, massaging the affected area. If the rear pouch is affected, painful sensations are possible when climbing or descending the stairs. Sometimes a minor local edema is noted. With suppuration of the bursa, the pain becomes sharp, twitching, baking, combined with hyperemia, edema of the affected area, symptoms of general intoxication.
- Tendinitis.Usually found in overweight men and athletes, it affects the own ligament of the kneecap. The pain syndrome initially only occurs with very intense exertion, then with normal sporting loads, then with daily physical activity or at rest. Pain with tendonitis is localized in front, just below the knee, dull, drawing, with the progression of the disease, sometimes paroxysmal, in some cases accompanied by a slight reddening and swelling, aggravated by pressure. Movement is usually complete, less often slightly restricted. A tear or breakage of the tape is possible due to a decrease in its strength.
- Lipoarthritis.Hoff's disease affects the layers of fat tissue that are under the kneecap. It is observed with constant overload of the knee or becomes the result of an old injury. More often it affects athletes, older women. A person complains of dull pain combined with some restriction in stretching. With the exacerbation of the pathology, the pain begins to bother at night, there is a feeling of instability of the knee, the bending of the leg. A faint cracking or creaking sound can be heard when the kneecap is pressed sideways.
Autoimmune processes
The cause of diseases of this group is the production of antibodies against the normal cells of the body with the development of immune complex aseptic inflammation of the synovial membrane and cartilage, the phenomena of vasculitis. Pathologies are in most cases chronic, without treatment they tend to progress and are often the cause of disability.
- Rheumatoid arthritis.The defeat is usually bilateral. With minimal activity of the autoimmune process, the pain is weak or moderate, intermittent, pulling, pressing, accompanied by morning stiffness. With moderate activity, the patient complains of periodically persistent aching, pressing or bursting pain of moderate intensity, not only during movement but also at rest. There is stiffness for many hours, moderate recurrent synovitis. With high activity of rheumatoid arthritis, the pain is severe, diffuse, exhausting, undulating and increases in the morning hours. The stiffness becomes constant, a large amount of fluid accumulates in the knees, contractures form over time.
- Systemic lupus erythematosus.Arthralgias are often symmetrical, although one joint can be affected. They can occur at any stage of the disease and are similar to rheumatoid arthritis in the case of a relapsing course of SLE. With little activity of the process, the pain is short-term, not intense, local, aching and pulling. In severe cases, the pain syndrome progresses, the pain is wavy, interferes with night sleep, becomes prolonged, diffuse, increases with movement, combined with synovitis, edema, hyperemia.
- Rheumatism.Joint pain is one of the first manifestations of rheumatic fever, occurs 5-15 days after an acute infection, affects several joints at the same time (usually paired). The pain is more short-term, but intense, wandering from one joint to another, differing in nature from pulling or pressing to burning or pulsing. The knees are swollen, hot, the skin above them is reddened. Movement is severely restricted. After a few days, the severity of the pain decreases, movements are restored. In some patients, residual effects in the form of moderate or mild dull pain persist for a long time.
- Reactive arthritis.Occurs more often 2-4 weeks after intestinal and genitourinary infections, usually affects one or two joints of the lower extremities, combined with urethritis, conjunctivitis. The development of reactive arthritis is preceded by increased urination, pain and burning in the urethra, tearing, and cramps in the eyes. Pain in the knee is severe or moderate, constant, wavy, aching, pulling, twitching, associated with restricted mobility, deterioration in general condition, fever, severe swelling and reddening of the affected area. Painful sensations and signs of inflammation last for 3 months to 1 year and then gradually go away.
Degenerative-dystrophic processes
They arise as a result of metabolic disorders in the structures of the joint and the periarticular soft tissues. They have a chronic course that progresses over many years. Often accompanied by the formation of calcifications, cysts and osteophytes, deformation of the surface of the knee. If the joint surfaces are severely damaged, they lead to a pronounced impairment of the movement and support functions, become the cause of disabilities and require the installation of an endoprosthesis.
- Arthrosis.It develops for no apparent reason or against the background of various injuries and diseases, especially in the elderly and middle-aged. The pain is initially weak, briefly, usually pulling or painful, occurs with prolonged exertion and disappears at rest, often accompanied by a crunch. Gradually, the pain syndrome worsens, the knees begin to hurt "in the weather" and movement is restricted at night. Signs of osteoarthritis of the knee are the onset of pain (it hurts until you "dissipate"), periodic attacks of sharp cuts, burning or stabbing pain due to the blockage. Often, during periods of exacerbation, synovitis occurs, with the pain becoming constant, oppressive, and bursting.
- Meniscopathy. . . Usually recognized in athletes whose work puts considerable strain on the knee joint. Manifested by unilateral local deep pain within the knee at the level of the joint space, more often in the outer half of the knee. The pain increases with movement and subsides at rest, it can be dull, pressing or pulling. With progression, acute stabbing pain occurs when trying to move. A small painful formation can sometimes be felt on the anterolateral surface of the joint when the pain is projected.
- Tendopathies. . . Tendons near the knees are affected. In the initial stage, they are manifested by short-term local superficial pain at the height of physical activity. Subsequently, painful sensations appear with moderate, and then light loads, which limit the usual daily activity. The pulling or aching pain that is directly associated with active movements is not felt during passive extension and flexion of the knee, sometimes accompanied by a crunch or crackle. In the area of the lesion, the most painful area can be probed. Local signs of inflammation (edema, hyperemia, hyperthermia) are insignificant or absent.
- Osteochondropathy.Children and adolescents are more often affected, the duration of the illness is several years. Usually they begin gradually with mild lameness or intermittent, non-intense dull pain that is aggravated with exertion and disappears with rest. As the osteochondropathy progresses, the pain becomes severe, constant, pressing, searing, or searing, accompanied by severe lameness, restricted mobility, and difficulty resting on the extremity. Then the pain gradually subsides and the support function is restored.
- Chondromatosis.Usually diagnosed in older men, less often in infants. Chondromatosis of the joints manifests itself as moderate dull, wavy pain that often worsens at night and in the morning. Movement is restricted, accompanied by a crunch. Sometimes blockages occur, which are characterized by sudden, stabbing pain, impossibility or severe restriction of movement. With the development of synovitis, the pain acquires a bursting character, associated with an increase in knee volume, swelling of the soft tissues and a local increase in temperature.
Tumors and tumor-like formations
The pain syndrome can be caused by a cyst, benign, or malignant tumor that directly affects the joint or periarticular tissue. In addition, knee pain can serve as an alarming signal for hypertrophic arthropathy, paracancrotic polyarthritis - paraneoplastic syndromes characteristic of lung cancer, breast cancer, and other oncological processes.
- Baker's cyst.Represents a hernia protrusion in the hollow of the knee. In the initial stage it manifests itself in unpleasant sensations or slight local pain along the hollow of the knee. Against the background of an increase in Baker's cyst due to compression of neighboring nerves, there may be burning or stabbing pain, numbness or tingling in the plantar area. Symptoms are worse when trying to bend the knee as much as possible. An elastic, slightly painful tumor-like formation can sometimes be felt in the popliteal fossa.
- Benign tumors.Includes chondromas, osteochondromas, non-ossifying fibromas, and other neoplasms. They are characterized by a longer asymptomatic or asymptomatic course, they can manifest themselves with vague and intermittent local, non-intense pain. With large neoplasms, a firm formation is felt, sometimes synovitis develops.
- Malignant neoplasms.The most common malignant tumors in the joint area are synovial sarcoma, osteosarcoma and chondrosarcoma. They manifest with dull, local, vague pain, sometimes with a certain circadian rhythm (worse at night). The intensity of pain increases, they become sharp, cutting, burning or twitching, spread along the knee and adjacent tissues, accompanied by deformations, edema, synovitis, expansion of the trunk veins, violation of the general condition, the formation of contractures. Upon palpation, a painful tumor-like formation is found. When the process begins, the pain is excruciating, excruciating, exhausting, depriving you of sleep, and not being eliminated by non-narcotic analgesics.
Invasive operations and manipulations
The pain syndrome is triggered by damage to the knee tissue during invasive interventions. The severity of the pain depends directly on the trauma of the manipulations on the knee joint. When pathogenic microbes enter the joint area, pain is caused by inflammatory changes.
- Manipulation.The most common procedure is puncture. Pain after the puncture is short-term, not intense, quickly subsides and is localized in the projection of the puncture, which is usually done on the outside of the knee. After a biopsy, the pain may twitch at first, then dull, and then go away after a few days.
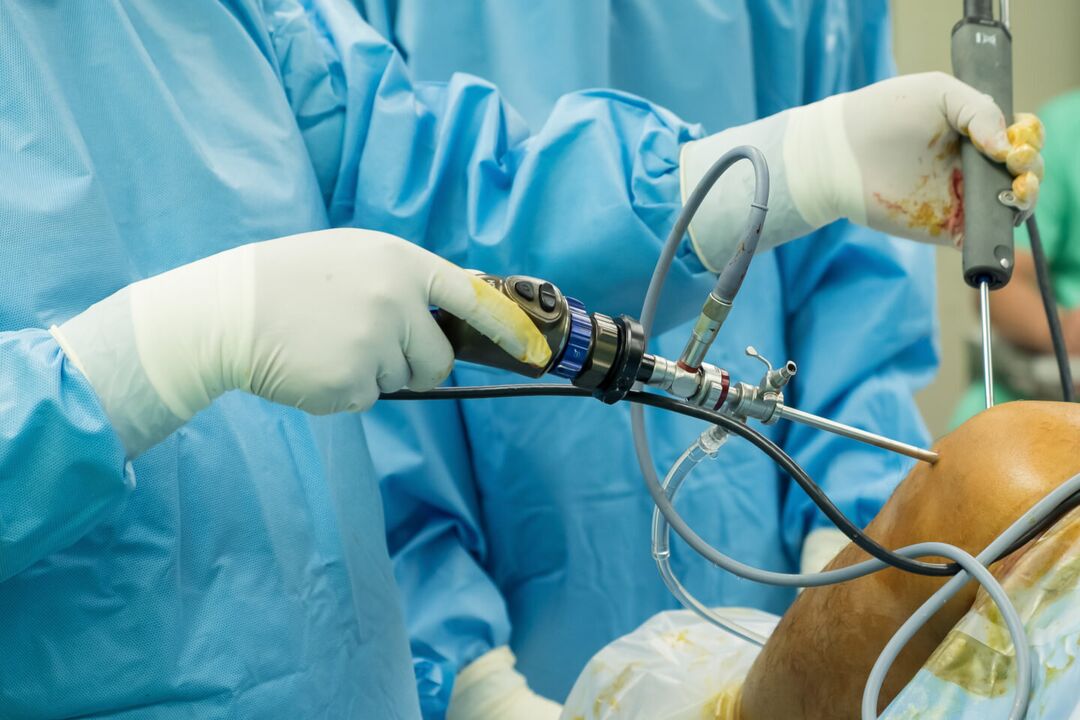
- Operations.After arthroscopy, the pain is moderate, initially quite acute, then dull and subsides after a few days or 1-2 weeks. After an arthrotomy, the pain syndrome is more intense; it can last for up to several weeks due to significant tissue damage. Usually, analgesics are prescribed to patients for the first 2 or 3 days after the procedures, then the pain becomes weak and gradually disappears.
Psychosomatic states
Sometimes arthralgia occurs in the knees without an organic basis (trauma, inflammation, destruction, etc. ) under the influence of psychological factors. Such pain is believed to have a protective role as it helps reduce emotional stress by converting experiences into physical sensations. A distinctive feature of such pain is its vagueness, inconsistency, the absence of visible changes, a clear association with physical activity and other objective provoking factors. Meteopathic arthralgias are seen in people who are sensitive to changes in air pressure.
In addition, radiation therapy for knee pain in coxarthrosis, lumbar osteochondrosis, Perthes disease, fibromyalgia, and sciatic nerve neuropathy is possible. However, with these pathologies, as a rule, pain syndromes of other localization come to the fore. Other risk factors that increase the likelihood of knee joint injuries and diseases are obesity, competitive sports, hypovitaminosis, metabolic disorders and age. Hypothermia, stress, physical exertion, and nutritional disorders can all be provoking factors that make chronic pain worse.
opinion poll
The diagnostic search algorithm is based on taking into account the type of pain syndrome, its duration and the identification of accompanying symptoms and events that precede the appearance of knee pain. At the first visit to the doctor (traumatologist-orthopedist, surgeon, rheumatologist), a visual examination and palpation of the knee, as well as an assessment of the volume of active and passive movements, are carried out. Taking into account the data received, the patient can be assigned in the future:
- Blood tests in the laboratory. . . A complete blood count will help identify hematological changes that are characteristic of an acute infectious and inflammatory process (leukocytosis, increased ESR), eosinophilia, which is typical of an allergic reaction. The most informative are biochemical and serological studies in autoimmune diseases, which are characterized by the formation of specific acute phase proteins and immunoglobulins (CRP, rheumatoid factor, ASL-O, CEC, antibodies against DNA, etc. ).
- Radiography.The basic diagnostic method is an X-ray of the knee joint in 2 projections. The presence of pathology is indicated by changes in the contours of the articular head and joint cavity, narrowing of the joint space, changes in the thickness of the end plates, the presence of edge defects at the joint ends of the bones, osteolysis and bone destruction. In some diseases (trauma to the meniscus, Baker's cyst), the contrast medium arthrography shows the greatest sensitivity.
- Osteoarthritis sonography. . . Knee ultrasound is a fast, inexpensive, inexpensive and very meaningful diagnostic method. Allows to assess the presence of effusion and free bodies in the joint cavity to identify damage and pathological changes in the periarticular soft tissues (signs of calcification, bleeding, etc. ). They help to differentiate the etiology of joint pain with high accuracy.
- CT and MRI. . . They are the method of choice for arthropathies of any origin. They are used to more precisely assess the type and extent of pathological changes in order to identify typical signs of traumatic, inflammatory and tumorous lesions of bone structures and soft tissues. CT and MRI of joints are usually used with limited informational content from other instrumental studies.
- Joint puncture. . . It is performed when there is evidence of the accumulation of exudate or transudate in the joint capsule. As part of the differential diagnosis of inflammatory, degenerative and tumor diseases, a cytological, bacteriological or immunological examination of the synovial fluid is carried out. To make the diagnosis of autoimmune damage to the knee joint, tuberculous arthritis, synovioma, it is extremely important to do a biopsy of the synovial membrane.
- Arthroscopy. . . The purpose of invasive endoscopic diagnostics can be the removal of a biopsy, the clarification of the necessary diagnostic information during a visual examination of joint elements. In some cases, diagnostic arthroscopy evolves into therapeutic (atroscopic removal of intra-articular bodies, menisectomy, autoplasty of ligaments, etc. ).
Symptomatic treatment
The treatment of the causes of knee pain is differentiated taking into account the identified disease. At the same time, symptomatic care is an essential part of a comprehensive treatment process that aims to alleviate symptoms and improve quality of life. Immediately after the injury, it is recommended to apply a cold compress to the knee area - this will help reduce sensitivity to pain. Ethyl chloride has a local cooling and anesthetic effect. In all cases, resting the knee will help reduce pain. It is necessary to limit movement, give the leg a position where pain is minimal. When walking, a fixation bandage is applied to the knee; the extremity can be immobilized with a plaster bandage.
In the acute phase of injury or illness, it is strictly forbidden to massage the knee, apply warming compresses and wear high-heeled shoes. The main classes of drugs for the symptomatic treatment of pain and inflammation are analgesics and NSAIDs in the form of ointments, tablets, and injections. The measures listed can only temporarily relieve the pain, but not eliminate the cause of the arthralgia. Therefore, all cases of knee pain require qualified diagnosis and treatment, and some diseases (fractures, dislocations, hemarthrosis) require emergency medical care. You can not postpone the visit to the doctor if the pain is associated with a change in the shape of the knee (swelling, smoothing of the contours, asymmetry), inability to perform flexion and extension movements, kneecap bulging, impairment of the support of the knee the limb.



























